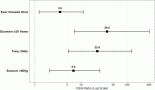
Cervical lesions have been associated with infection by high-risk human papilloma virus (high-risk HPV). In 409 women aged >15 years high-risk HPV lesions were identified. In a cohort of this population persistent infection was compared with cytological, colposcopic, and histological lesions. Cervical scrapes were taken and DNA was isolated. HPV was detected by PCR in the E6/E7 region. Genotyping was performed by PCR nested multiple E6/E7. HPV was detected in a 37.40% (153/409), high-risk HPV in 86% (153/178), HPV18 46.64% (83/178), HPV16 34.28% (61/178). Among these 53.93% (96/178) were multiple infections, and HPV18/16 (30/96) was the most frequent 31.25%. The cytology showed changes in 15% of positive patients. A 49.67% in women positive for HPV infection showed abnormalities in the colposcopic study, a relationship that turned out to be statistically significant ( p < 0.0019 test χ2). Among all 85% of the women were younger than 45 years of age. Fifty-seven patients were evaluated 15 months after the base study, with initial prevalence of morbidity 49.12% (28/57) and at the end 10.53% (6/57), showing in 89.29% (25/28) negative for HR-HPV infection, 10.34% (3/28) showed persistence of infection, 17.54% (10/57) presented cytological alterations, with 80% of positivity for HPV, and a regression of 100% (10/10) of the previously identified lesions. With colposcopy, 50% (14/28) presented alterations related to HPV, of these 85.71% (12/14) showed regression of such an alteration. The cumulative incidence for HPV was 10.34% (3/29). The incidence rate was 4.23% (3/71), which is equal to 4.23 new cases of HPV infection per 100 people, per year of follow-up. In conclusion, the present work shows a high frequency of infection by high-risk HPV, with predominance of HPV18 and 16 and in general for multiple infections. Colposcopy was better predictor than the Pap smear for infection. The follow-up study revealed a low percentage of persistent infection, and a high frequency of negativity for viral infection, high regression of cytological and colposcopic lesions, a low cumulative and incidence rate similar to that reported by other Latin American countries and higher than the European countries.