Patient-centred care: a scoping review of measures of patient centredness in healthcare in low- and middle-income countries (LMICs)
Anna Cabanes1, Cindy Sun1, Diksha Thakkar1, Carolyn Taylor1 and Phuong Thao Le2
1Global Focus on Cancer, South Salem, NY 10590, USA
2Boston University School of Public Health, Boston University, Boston, MA 02215, USA
Abstract
Person- or patient centredness (PC) is increasingly recognized as a core component of high-quality healthcare and a critical pathway to achieving equitable, person-responsive cancer services. While the concept of PC has been widely adopted and measured in high-income countries, its implementation and evaluation in low- and middle-income countries (LMICs) remain limited and inconsistent. This scoping review maps existing research on measures of PC in LMICs, with a specific focus on cancer care. We identified 345 studies published between 2004 and 2022 that reported on PC in LMICs, of which 20 focused on cancer. Most studies were conducted in upper-middle-income countries and used cross-sectional designs. Patient satisfaction was the most commonly measured domain, followed by communication and shared decision-making. However, foundational aspects of PC – such as patient rights, coordination of care and culturally responsive services – were rarely evaluated. Only 41% of studies used validated tools, and most interventions occurred at the facility level, with few system-level evaluations. Using the Santana et al. framework, which categorizes PC domains into structure, process and outcomes, we found that structural and systemic components of PC were particularly underrepresented in LMIC research. This suggests a gap between policy ambitions and practical implementation, especially in cancer care settings where multidisciplinary coordination and patient engagement are essential. This review advances the field by systematically documenting how PC is currently measured in LMICs and identifying significant limitations in scope, equity and contextual relevance. Findings highlight the urgent need for validated, culturally adaptable tools and frameworks that reflect the realities of LMIC health systems. Addressing these gaps is essential for scaling person-centred cancer care and strengthening health systems toward universal health coverage.
Keywords: person-centred care, patient-centred care, people-centred care, LMIC, indicator
Correspondence to: Anna Cabanes
Email: anna@globalfocusoncancer.org
Published: 27/03/2026
Received: 05/06/2025
Publication costs for this article were supported by ecancer (UK Charity number 1176307).
Copyright: © the authors; licensee ecancermedicalscience. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Background
People-centred, person-centred and patient-centred healthcare systems respect the experience, values, needs and preferences of people in the planning, coordination and delivery of care. People-centred care looks at communities, person-centred care looks at the whole individual and patient-centred care (PCC) looks at the person specifically as a patient receiving treatment.
The concept of patient-centredness (PC) is not new, but its implementation has primarily been concentrated in high-income countries (HICs) and has been shown to improve patient outcomes, optimize resource utilisation, reduce costs and enhance satisfaction with care [1]. In 2018, three major reports emphasized PC as a cornerstone for enhancing the quality of healthcare systems across all resource levels, an essential component of functional health systems and a vital mechanism for achieving equitable access to quality care through universal health coverage [2–4].
Despite the recent extensive body of research and the prominence of PC in policy discussions, the concept lacks a universally accepted definition. An analysis of existing theoretical frameworks reveals multiple models, each emphasising different dimensions of PCC, for example, patient-provider relationship and communication (COM), integration of medical and non-medical care, coordination and continuity of care, patient participation and involvement of family and friends, among others [5–9]. These are understood and applied differently across contexts and among diverse stakeholders, which impacts the effective implementation and evaluation of patient-centred initiatives.
Among the frameworks reviewed, the model proposed by Santana et al [8] stands out for its practical applicability. This framework integrates the components of PC into the Donabedian model for healthcare improvement [10], categorising them into structure, process and outcomes for practical implementation in healthcare systems.
Figure 1 presents the conceptual framework adapted from Santana et al [8]. Structure domains encompass aspects of PCC at both foundational (healthcare system) and organisational levels. Process domains include four subdomains focused on the interactions between patients and healthcare providers. Outcome addresses two domains centred on patient experience (PE) and health outcomes. Measuring the impact of PC requires the use of appropriate indicators to assess its quality. By breaking PC into these distinct components, this framework provides a solid foundation for evaluation and quality improvement.
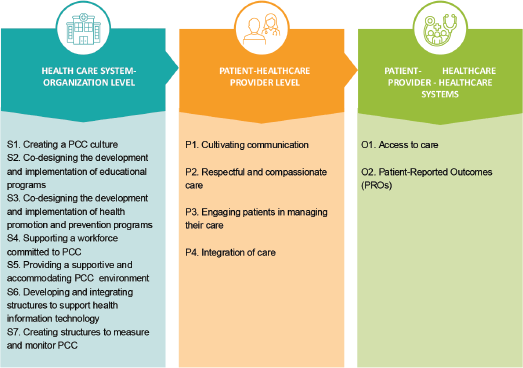
Figure 1. Conceptual framework for PCC adapted from Santana et al [8].
The challenge of measuring PC is reflected in the diverse array of tools developed, tested and applied across various settings [8, 11]. While some tools aim to comprehensively evaluate PC, many focus on specific aspects of the concept. Certain tools are designed to measure PC over time, while others assess it within the scope of a single healthcare visit. Additionally, some tools are designed for use within individual facilities, whereas others can be applied across entire healthcare systems.
The most commonly measured domains include patient perceptions of PC [12], patient-reported experiences [13], fostering a PC culture, physician-patient COM [6, 14–17] and shared decision making (SDM) [5], among others. However, the majority of these studies have been conducted in HICs.
In low- and middle-income countries (LMICs), there is growing recognition of the importance of PC, but significant challenges persist in assessing its impact [18–20]. While frameworks and tools for measuring PC are established in high-income settings, their applicability in LMICs is often limited by contextual differences. Existing tools may not adequately capture the unique sociocultural, economic and systemic factors that shape healthcare experiences in these regions. For example, variations in health literacy, resource constraints and distinct patient-provider dynamics often necessitate adaptation and validation of PC measurement instruments.
Efforts are required to develop and validate tools that accurately reflect the realities of LMIC healthcare systems. Context-specific research is essential to create standardized yet adaptable approaches for evaluating PC in these settings. Such tools should accommodate the challenges of limited resources while providing reliable and actionable insights to improve healthcare delivery.
This scoping review aimed to identify measures of PC used in LMIC contexts and analyse a valid set of indicators suitable for resource-constrained settings. While the scoping review was not limited to a specific disease type, we conducted a sub-analysis of articles focused on cancer, aligning with the primary focus of our work.
Methods
Search strategy
This study followed PRISMA guidelines for scoping reviews [21]. Keywords were developed by reviewing published literature for terms related to people-centred, people-focused, patient-centred and patient-focused care, as well as countries categorized as low income, lower-middle income or upper-middle income according to the 2022 World Bank classification (https://datatopics.worldbank.org/world-development-indicators/the-world-by-income-and-region.html).
We searched the following databases: PubMed, ERIC and CINAHL and restricted articles to those published in English between January 2004 and December 2022. Data collection and analysis were conducted from January through July 2023.
Inclusion/exclusion criteria
Articles were included in this review if they were original research studies focused on measuring PCC or any of its domains and were implemented in LMICs. The review included articles across all disease and care settings within LMICs.
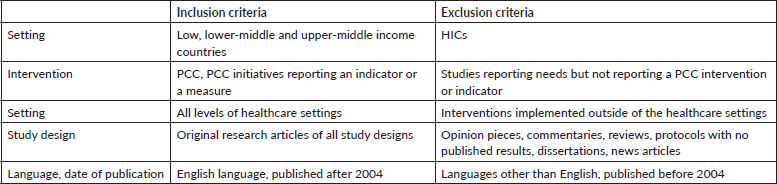
Articles were excluded from this review if they did not report indicators or measures, were conducted in a HIC, were published in a language other than English, lacked full-text availability or were conference abstracts. We excluded studies in which some components of PC were evaluated but not in relation to PC. For example, studies measuring satisfaction with surgical outcomes solely based on clinical results were not included. Table 1 illustrates the inclusion and exclusion criteria applied during the screening process.
Table 1. Inclusion and exclusion criteria.
Data extraction and assessment of quality
The initial search retrieved 1,219 articles. After removing duplicates, 1,144 articles were selected for screening. Three research team members conducted a two-phase screening process for each selected article. Each article was reviewed by two people (DT, CS), with a third reviewer (AC) resolving disagreements through consensus. This process resulted in the exclusion of 547 articles. A subsequent full-text review resulted in the exclusion of an additional 252 articles for not specifically evaluating the interventions.
After screening, 345 articles were included in this review. Figure 2 presents the PRISMA flow diagram illustrating the selection process. Two members of the review team extracted key information from each article, including: title, lead author, year of publication, study country and resource level, whether the study was conducted in the general patient population or directed to a specific disease, intervention details, study outcome, healthcare system level; study design, whether there was a control group and the number of participants; the general domain of PC being measured; the tools used to measure it and whether the tool or instrument had been previously validated, was validated in the study or was not validated. We sought to extract all the fields listed above for each article. However, in some cases, studies did not report all the variables. We followed the Synthesis Without Meta-analysis reporting guidelines (https://swim.sphsu.gla.ac.uk/) for reporting of the results.
Note that, for clarity throughout the review, we use PC as the overarching concept and PCC as a specific subdomain for which measurement tools have been developed.
Results
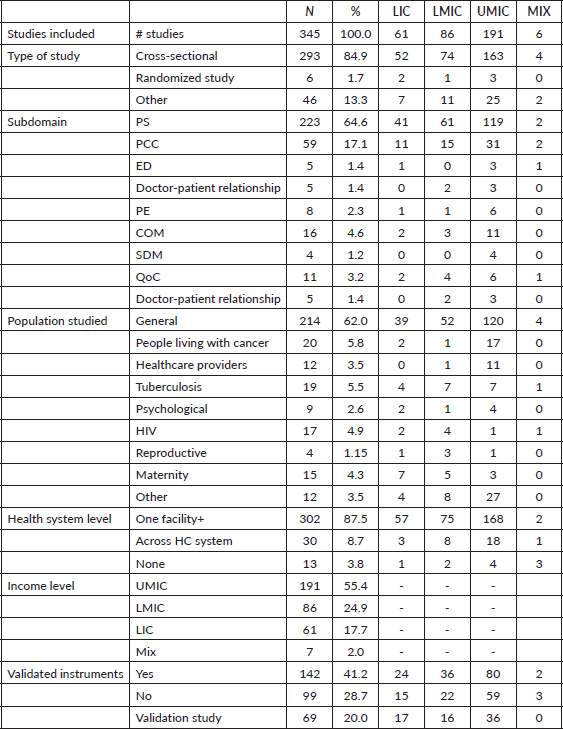
A total of 345 studies were included in the review, reporting measures of PC in LMICs. The number of articles on PC measures progressively increased from 2004 through 2022, peaking in 2021. Table 2 summarizes the characteristics of the studies included.
Income levels of the countries in the included studies
Of the 345 selected studies, 191 (55%) articles were conducted in upper-middle income countries, 86 (25%) in LMICs and 61 (18%) in low-income countries (six studies were implemented in several countries with varying income levels). The countries with the most studies included were China (n = 72), Ethiopia (n = 37), Turkey (n = 24), Malaysia (n = 23) and Nigeria (n = 16). Table 3 shows the five countries of each income level group with more articles included, and the number of articles from each.
Study design
293 studies used a cross-sectional study design, 6 utilized randomized control trial design and 3 were cohort studies. There was no control group in 323 studies, whereas 15 studies included a control group. The total number of participants in the studies varied from 17 to 83,046. Study subjects varied from nurses, physicians, patients, medical providers, to facilities and districts also surveyed.
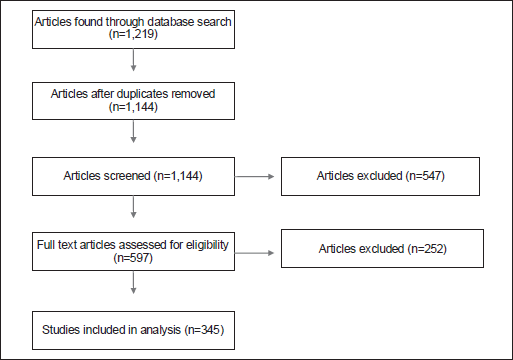
Figure 2. PRISMA flow diagram.
Of the 6 RCT, only two studies targeted family/PC, 3 assessed satisfaction as a secondary outcome of a non-patient centred intervention, and one used quantitative data from a randomized control trial and offered descriptive analysis without an intervention [22].
Population under study
Most studies focused on measuring PCC in the general patient population (n = 214), compared to other patient groups. After the general patient population, people living with cancer (n = 20), with tuberculosis (n = 19), and HIV/AIDS (n = 17) or attending maternal health services (n = 15) were most often analysed. Healthcare providers were included in 12 articles. Among the articles focused on cancer, breast, colorectal, hepatocellular, lung, liver and hematologic cancers were most frequently studied.
Level/s of the healthcare system where the intervention was implemented
Of the studies reviewed, 302 implemented the intervention at the health facility level (one or more facilities), and 30 were conducted across the health system. Thirteen studies (n = 13) were categorized as ‘other’, including interventions implemented in pharmacies, dialysis centers or other healthcare-related facilities.
Measuring different PC domains
The elements of PC most frequently evaluated were patient satisfaction (PS) (n = 223), PCC (n = 59), patient provider COM (n = 16) and PE (n = 8). Other key domains of PC, such as patients' rights (0%), quality of life (<5%), SDM (3.3%) and multidisciplinary care, were never or seldom measured.
Table 2. Characteristics of studies included in the scoping review by country income level.
Measuring PC at the facility level
Most frequently, PC was measured at one facility or several facilities (n = 302). These facilities were primary level facilities (n = 83), and tertiary level or specialized care facilities (n = 90). Nineteen articles were implemented at secondary level facilities or general hospitals (GHs) (n = 84). Table 4 presents the distribution of specific PCC domains across different healthcare levels: primary, secondary, tertiary and GH/district.
PS was the most frequently analysed domain across all healthcare levels, followed by PCC. Quality of care (QoC) was assessed across all levels, with the highest proportion observed at the secondary care level (5.3%), while education (ED) was reported in both secondary (5.3%) and GH/District levels (3.6%), but not in other levels. As expected, SDM was primarily reported at the tertiary care level (3.3%), where more specialized and complex care decisions are typically made.
Measuring PC across the healthcare system
Thirty studies assessed PCC across a healthcare system. Of these, a third (n = 10) used validated tools. Countries included in these studies are China, Kenya, Lebanon, Pakistan and Turkey.
The validated tools used to assess PC included the European Patients Evaluate General/Family Practice PS survey [23, 24]; an adapted Chinese version of Hospital Consumer Assessment of Healthcare Providers and Systems [25], the World Health Organisation SAGE [26], SERVQUAL tool [27], the Person-centred Maternity Care Scale [28] and the Picker Patient Experience Questionnaire [29]. Additionally, two tools were validated during the studies; an adapted version of the Commonwealth Fund [30] and Harris Interactive Questionnaire [30] used in multiple countries, including Brazil, Colombia, Mexico and El Salvador; and the 1998 Kaiser National Household Survey [31], a client satisfaction tool validated in a study conducted in South Africa. Several other tools were used in health system-wide studies but were not validated.
Table 3. Number of articles in the top five countries per income level group.
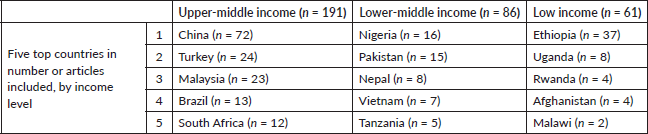
Table 4. Specific PC domains addressed in the included articles across different healthcare levels.
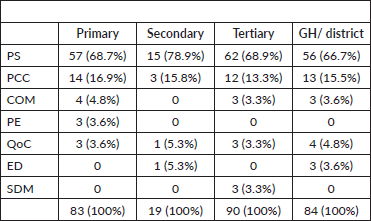
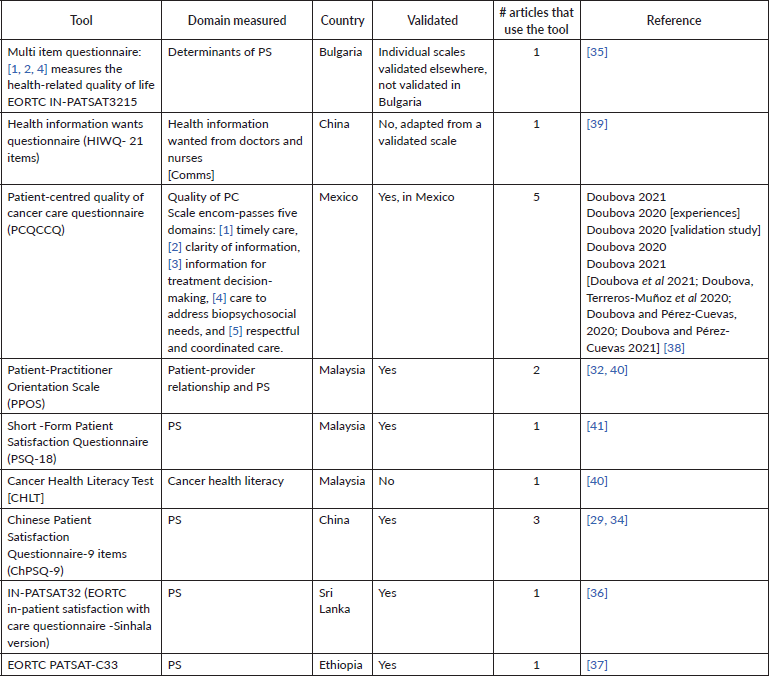
Table 5. Most common validated tools used to assess PC in cancer.
QoC, SDM, doctor-patient relationships and COM, and patient ED. However, other domains and subdomains of cancer PC were not measured. Notably, seventy percent of the articles measuring PC in cancer utilized validated tools.
Certain domains of PC, such as PS and QoC, are commonly assessed using a variety of measurement tools. In some cases, these domains are evaluated with a single tool that captures specific aspects of the PE. However, more comprehensive evaluations may use composite measures that combine several scales to provide a broader understanding of the determinants of PS and care quality. These composite measures might integrate factors like COM effectiveness, emotional support, respect for patient preferences and coordination of care, offering a more nuanced view of how well healthcare services align with the principles of PC.
Among the 20 reviewed articles focused on cancer, 8 assessed PS using validated instruments. Four of these studies used generic measures, specifically the Patient Satisfaction Questionnaire short forms (PSQ-9 or PSQ-18) [29, 32–34], while the remaining four employed cancer-specific tools from the EORTC PATSAT family, including inpatient (IN-PATSAT32) and outpatient (OUT-PATSAT33/PATSAT-C33) versions or related adaptations [35–38]. Thus, PS in cancer care was measured using a mix of generic and oncology-specific instruments across studies.
Discussion
In LMICs, significant gaps remain in the evaluation of PCC. Most studies in these settings focus on a limited range of measures, primarily assessing PS rather than the broader domains of PC. While several studies have examined PC within specific geographic regions, there is a lack of research identifying appropriate indicators and instruments tailored to regional healthcare contexts. To the best of our knowledge, our study is the first to assess measures of PC across countries of different income levels.
For instance, a systematic literature review by Alkhaibari et al [18] identified key elements of PC in the Middle East and North Africa, and suggests that PC is only partially practiced and supported in the region, with cultural factors significantly influencing its implementation. This review emphasizes the need for a regionally relevant definition of PC that incorporates cultural nuances and underscores the importance of considering these cultural dynamics when designing and implementing PC strategies.
Similarly, a scoping review exploring PC in Latin America revealed considerable variation across countries in their emphasis on PC versus family-centred care (FCC): among the 32 studies analysed, nearly half were conducted in Brazil. The review found that patient information was the most highlighted dimension of PC, while physical support received the least emphasis [20].
In sub-Saharan Africa, a study identified seven key themes of PC: patient provider COM, understanding, respect, compassion, stigmatisation, decision-making and trust [19]. This review highlighted significant challenges such as poor COM and mistreatment in patient-provider interactions, recommending targeted training programmes for healthcare providers to enhance PC practices.
The three studies share a common focus on PC within specific geographic regions and underscore the need for culturally tailored approaches to PC implementation. Despite regional differences, all studies stress the lack of standardized indicators for evaluating PC and emphasize the need for frameworks that address cultural and systemic nuances.
To analyse our scoping review, we adopted Santana's conceptual framework which offers a structured roadmap for guiding healthcare systems and organisations in delivering PC [8]. This framework applies the Donabedian model to characterize PC domains into three main groups: structure, process and outcome. Structure domains pertain to the healthcare system or the context in which care is provided, forming the foundation for PC. Process domains focus on the interactions between patients and healthcare providers, while outcome domains reflect the tangible results of PC, demonstrating its value through measurable impacts such as PS and experience.
Most of the articles we reviewed primarily focus on measuring single aspects/dimensions of PC, such as PS and PE. However, effective PC implementation requires attention to the structural aspects of healthcare systems, such as integrating PC principles into professional ED and fostering meaningful partnerships with patients and patient organisations. It also necessitates strong process elements that enhance patient-provider interactions. Despite their importance, our review found that these critical structural and process domains are rarely measured in LMICs, highlighting a significant gap in the evaluation and implementation of PC in these settings.
Additionally, we found that PS and PE are measured inconsistently across studies and settings. In some cases, PS is assessed as a single variable using a straightforward yes/no scale or a numerical scale. While this approach provides a quick snapshot of satisfaction, it may fail to capture the nuances of PEs, such as how well their specific needs were addressed or how they perceived COM with their provider.
In contrast, other studies measure PS as a composite variable encompassing multiple dimensions of care. These dimensions may include COM quality, timeliness of services, respect for patient preferences, physical comfort and emotional support.
Across the six studies that reported a RCT design, the ones reporting person- and family-centred approaches generally improved patient or caregiver experience, and, in several cases, strengthened clinical outcomes, with the strongest effects seen in interventions designed to enhance COM or family involvement [42, 43]. The studies focused on patient-centred COM in Uganda and family centred neonatal care in China, demonstrated clear, statistically significant gains, while simple behavioural nudges like reminder calls also improved the quality of the intervention and satisfaction [44]. In contrast, large system or policy changes resulted in more variable effects on satisfaction [45, 46]. This underscored that patient-centred benefits may be better assessed in studies explicitly designed to strengthen patient/FCC rather than as a secondary or downstream outcome of a non–patient-centred intervention.
Regarding the measurement of patient-centred cancer care, we found a limited focus on cancer patients. While many studies measured PC in general patient populations, only 20 articles specifically examined PC in oncology-targeted cancer patients. This highlights a significant gap in the literature, suggesting that the unique needs and challenges of implementing PC in cancer care remain underexplored and may require greater attention in future research.
Most interventions measuring PC in cancer originated from upper-middle income countries, possibly reflecting emerging healthcare reforms or targeted investments in quality of oncology care in these economies. A notable proportion (70%) of studies used validated tools, which is encouraging for the reliability of their findings. However, the limited scope of domains assessed, and the variability of instruments used, suggests that existing tools may not comprehensively capture all elements of PC relevant to cancer care.
For example, most studies used validated PS instruments, supporting the credibility and internal validity of the findings. However, the split between generic PSQ tools and cancer-specific EORTC PATSAT measures introduces heterogeneity that limits direct comparability across studies and complicates synthesis. While PSQ instruments offer feasibility and cross-setting comparability, the EORTC PATSAT scales provide greater sensitivity to oncology-specific care processes and setting-specific experiences. This variability highlights an ongoing tension between feasibility and specificity in PE measurement and underscores the need for greater alignment around core patient-centred metrics in cancer research. For policymakers and implementers, this trade-off highlights the need to balance how easy it is to compare results and the effort required to collect data with the level of detail needed to improve cancer services.
Conclusion
In summary, our findings reveal significant gaps in the literature regarding PC in LMICs, particularly in terms of the comprehensiveness of assessed domains and the geographic distribution of studies. Future research should aim to broaden the scope of PC evaluations to include underrepresented domains and settings and expand studies to low-income countries where data remains limited. Additionally, developing or adapting validated measurement tools tailored to specific healthcare settings could provide more robust insights into the delivery and impact of PC in these settings.
This study provides a snapshot of the use of standardized measures of PCC in LMICs, using Santana’s framework of structure, process, and outcome domains. To the best of our knowledge, our study is the first to assess measures of PC across countries of different income levels. However, a key limitation of the study is the heterogenous use of the term ‘PCC’, which led to a retrieval of a wide variety of scales and tools, making it challenging to draw clear conclusions. Future research should focus on specific aspects of PCC, particularly foundational domains or disease-specific dimensions, to enhance the precision and applicability of measurement approaches.
List of abbreviations
CHLT, Cancer health literacy test; COM, Communication; ED, Education; EORTC, European Organisation for Research and Treatment of Cancer; FCC, Family-centred care; GH, General hospital; HICs, High-income countries; IN-PATSAT32, In-patient satisfaction with care questionnaire [32-item scale developed by EORTC]; LIC, Low-income country; LMICs, Low- and middle-income countries; PCC, Patient-centred care; PE, Patient experience; PPOS, Patient-Practitioner Orientation Scale PRISMA, Preferred Reporting Items for Systematic Reviews and Meta-Analyses; PSQ-18, Patient satisfaction questionnaire [18-item short form]; QoC, Quality of care; SDM, Shared decision-making; SERVQUAL, Service quality [an instrument to measure service quality]; UMIC, Upper-middle income country; WHO SAGE, World Health Organisation Study on Global AGEing and Adult Health.
Conflicts of interest
The authors have no conflicts of interest to declare that are relevant to the content of this article.
Funding
The authors did not receive support from any organisation for the submitted work.
Informed consent
Not applicable.
Author contributions
AC, CT, PTL developed the concept and design. AC, CS and DT worked in acquisition of data and reviewed the included articles. All authors made substantial analysis and interpretation of data; drafted and revised the article for important intellectual content; and have seen and approved the final version of the manuscript.
References
1. Kohl S (2018) OECD—delivering quality health services: a global imperative Eur J Hosp Pharm 25(5) 286–288 https://doi.org/10.1136/ejhpharm-2018-001692
2. Bau I, Logan RA, and Dezii C, et al (2019) Patient-centered, integrated health care quality measures could improve health literacy, language access, and cultural competence NAM Perspect [Internet] [https://nam.edu/patient-centered-integrated-health-care-quality-measures-could-improve-health-literacy-language-access-and-cultural-competence/] Date accessed: 18/11/2024 https://doi.org/10.31478/201902a
3. Kieny M-P and Evans, TG (2018) Delivering quality health services: a global imperative for universal health coverage. [Internet] (Washington, D.C.: World Bank Group)
4. Kruk ME, Gage AD, and Arsenault C, et al (2018) High-quality health systems in the Sustainable Development Goals era: time for a revolution Lancet Glob Health 6(11) e1196–e1252 https://doi.org/10.1016/S2214-109X(18)30386-3 PMID: 30196093 PMCID: 7734391
5. Gartner JB, Abasse KS, and Bergeron F, et al (2022) Definition and conceptualization of the patient-centered care pathway, a proposed integrative framework for consensus: a Concept analysis and systematic review BMC Health Serv Res 22 558 https://doi.org/10.1186/s12913-022-07960-0 PMID: 35473632 PMCID: 9040248
6. Mead N and Bower P (2000) Patient-centredness: a conceptual framework and review of the empirical literature Social Sci & Med 51(7) 1087–1110 https://doi.org/10.1016/S0277-9536(00)00098-8
7. Olson AW and Burns AL (2023) From patient centered to person centered: the pharmacist’s role and value in community-integrated care transformation J Am Pharm Assoc 63(3) 736–741 https://doi.org/10.1016/j.japh.2023.03.003
8. Santana MJ, Manalili K, and Jolley RJ, et al (2018) How to practice person‐centred care: a conceptual framework Health Expect Int J Public Particip Health Care Health Policy 21(2) 429–440
9. Scholl I, Zill JM, and Härter M, et al (2014) An Integrative Model of Patient-Centeredness – A Systematic Review and Concept Analysis PLoS One 17(9) e107828 https://doi.org/10.1371/journal.pone.0107828
10. Donabedian A (1988) The quality of care. How can it be assessed? JAMA 23(12) 1743–1748 https://doi.org/10.1001/jama.1988.03410120089033
11. Louw JM, Marcus TS, and Hugo J (2020) How to measure person-centred practice - An analysis of reviews of the literature Afr J Prim Health Care Fam Med 12(1) e1–e8 https://doi.org/10.4102/phcfm.v12i1.2170 PMID: 32129646 PMCID: 7136800
12. Hudon C, Fortin M, and Haggerty JL, et al (2011) Measuring patients’ perceptions of patient-centered care: a systematic review of tools for family medicine Ann Fam Med 9(2) 155–164 https://doi.org/10.1370/afm.1226 PMID: 21403143 PMCID: 3056864
13. Patient-Centred Healthcare Indicators Review [Internet]. (2012) International Alliance of Patient’s Organizations [https://www.iapo.org.uk/sites/default/files/files/IAPO%20Patient-Centred%20Healthcare%20Indicators%20Review.pdf]
14. Brouwers M, Rasenberg E, and Van Weel C, et al (2017) Assessing patient-centred communication in teaching: a systematic review of instruments Med Educ 51(11) 1103–1117 https://doi.org/10.1111/medu.13375 PMID: 28762538 PMCID: 5655924
15. Lewis S (2009) Patient-Centered Care: An Introduction to What It Is and How to Achieve It A Discussion Paper for the Saskatchewan Ministry of Health Ministry of Health, Saskatchewan, Canada
16. Sustersic M, Gauchet A, and Kernou A, et al (2018) A scale assessing doctor-patient communication in a context of acute conditions based on a systematic review PLoS One 13(2) 192306 https://doi.org/10.1371/journal.pone.0192306
17. Zill JM, Christalle E, and Müller E, et al (2014) Measurement of physician-patient communication--a systematic review PLoS One 9(12) e112637 https://doi.org/10.1371/journal.pone.0112637 PMID: 25532118 PMCID: 4273948
18. Alkhaibari RA, Smith-Merry J, and Forsyth R, et al (2023) Patient-centered care in the Middle East and North African region: a systematic literature review BMC Health Serv Res 23 135 https://doi.org/10.1186/s12913-023-09132-0 PMID: 36759898 PMCID: 9909864
19. Camara BS, Belaid L, and Manet H, et al (2020) What do we know about patient-provider interactions in sub-Saharan Africa? A scoping review Pan Afr Med J 37 88 https://doi.org/10.11604/pamj.2020.37.88.24009 PMID: 33244351 PMCID: 7680249
20. Klimesch A, Martinez‐Pereira A, and Topf C, et al (2023) Conceptualization of patient‐centered care in Latin America: a scoping review Health Expect Int J Public Particip Health Care Health Policy 26(5) 1820–1831
21. Tricco AC, Lillie E, and Zarin W, et al (2018) PRISMA Extension for Scoping Reviews (PRISMA-ScR): checklist and Explanation [Internet] Ann Intern Med Internet 2021 [https://www.acpjournals.org/doi/abs/10.7326/M18-0850]
22. Miller P, Afulani PA, and Musange S, et al (2021) Person-centered antenatal care and associated factors in Rwanda: a secondary analysis of program data BMC Pregnancy Childbirth 21(1) 290 https://doi.org/10.1186/s12884-021-03747-z PMID: 33838658 PMCID: 8037834
23. Gorgulu O (2018) Determination of the relationship between patient satisfaction and some global economic indicators using multidimensional scaling Niger J Clin Pract 21(11) 1422–1429 https://doi.org/10.4103/njcp.njcp_218_17 PMID: 30417839
24. Sparkes SP, Atun R, and Bӓrnighausen T (2019) The impact of the Family Medicine Model on patient satisfaction in Turkey: panel analysis with province fixed effects PLoS One 14(1) 210563 https://doi.org/10.1371/journal.pone.0210563
25. Liang H, Xue Y, and Zhang ZR (2021) Patient satisfaction in China: a national survey of inpatients and outpatients BMJ Open 7(9) 49570
26. Alshamsan R, Lee JT, and Rana S, et al (2017) Comparative health system performance in six middle-income countries: cross-sectional analysis using World Health Organization study of global ageing and health J R Soc Med 110(9) 365–375 https://doi.org/10.1177/0141076817724599 PMID: 28895493 PMCID: 5987910
27. Haj-Ali W, Bou Karroum L, and Natafgi N, et al (2014) Exploring the relationship between accreditation and patient satisfaction - the case of selected Lebanese hospitals Int J Health Policy Manag 3(6) 341–346 https://doi.org/10.15171/ijhpm.2014.116 PMID: 25396210 PMCID: 4226624
28. Oluoch-Aridi J, Afulani P, and Makanga C, et al (2021) Examining person-centered maternity care in a peri-urban setting in Embakasi, Nairobi, Kenya PLoS One 16(10) 257542 https://doi.org/10.1371/journal.pone.0257542
29. Wong WS, Fielding R, and Wong C, et al (2009) Confirmatory factor analysis and sample invariance of the Chinese Patient Satisfaction Questionnaire (ChPSQ-9) among patients with breast and lung cancer Value Health J Int Soc Pharmacoeconomics Outcomes Res 12(4) 597–605 https://doi.org/10.1111/j.1524-4733.2008.00480.x
30. Doubova SV, Guanais FC, and Pérez-Cuevas R, et al (2016) Attributes of patient-centered primary care associated with the public perception of good healthcare quality in Brazil, Colombia, Mexico and El Salvador Health Policy Plan 31(7) 834–843 https://doi.org/10.1093/heapol/czv139 PMID: 26874326
31. Myburgh NG, Solanki GC, and Smith MJ, et al (2005) Patient satisfaction with health care providers in South Africa: the influences of race and socioeconomic status Int J Qual Health Care J Int Soc Qual Health Care 17(6) 473–477 https://doi.org/10.1093/intqhc/mzi062
32. Chan CM and Azman WA (2012) Attitudes and role orientations on doctor-patient fit and patient satisfaction in cancer care Singap Med J 53(1) 52–56
33. Wong WS, Fielding R, and Wong CM, et al (2008) Psychometric properties of the Nine-Item Chinese Patient Satisfaction Questionnaire (ChPSQ-9) in Chinese patients with hepatocellular carcinoma Psychooncology 17(3) 292–299 https://doi.org/10.1002/pon.1247
34. Lam WWT, Kwong A, and Suen D, et al (2018) Factors predicting patient satisfaction in women with advanced breast cancer: a prospective study BMC Cancer 18(1) 162 https://doi.org/10.1186/s12885-018-4085-3 PMID: 29415669 PMCID: 5803988
35. Djambazov SN, Giammanco MD, and Gitto L (2019) Factors That Predict Overall Patient Satisfaction With Oncology Hospital Care in Bulgaria Value Health Reg Issues 19 26–33 https://doi.org/10.1016/j.vhri.2018.11.006 PMID: 30641294
36. Jayasekara H, Rajapaksa L, and Bredart A (2008) Psychometric evaluation of the European Organization for Research and Treatment of Cancer in-patient satisfaction with care questionnaire (“Sinhala” version) for use in a South-Asian setting Int J Qual Health Care J Int Soc Qual Health Care 20(3) 221–226 https://doi.org/10.1093/intqhc/mzn006
37. Abate D, Aman MA, and Nasir BB, et al (2020) Assessment of quality of care using information on patient satisfaction at Adult Oncology Center of Tikur Anbessa specialized Hospital, Ethiopia: a Cross-Sectional Study Patient Prefer Adherence 14 847–858 https://doi.org/10.2147/PPA.S253027 PMID: 32546979 PMCID: 7247603
38. Doubova SV, Martinez-Vega IP, and Gutiérrez-De-La-Barrera M, et al (2020) Psychometric validation of a Patient-Centred Quality of Cancer Care Questionnaire in Mexico BMJ Open 10(3) 33114 https://doi.org/10.1136/bmjopen-2019-033114
39. Xie B, Su Z, and Liu Y, et al (2015) Health information wanted and obtained from doctors/nurses: a comparison of Chinese cancer patients and family caregivers Support Care Cancer Off J Multinatl Assoc Support Care Cancer 23(10) 2873–2880
40. Chan CMH, Blanch-Hartigan D, and Taib NA, et al (2020) Preferences for patient-centered care among cancer survivors 5 years post-diagnosis Patient Educ Couns 103(8) 1601–1605 https://doi.org/10.1016/j.pec.2020.02.033 PMID: 32143985
41. Ahmed S, Djurkovic A, and Manalili K, et al (2019) A qualitative study on measuring patient-centered care: perspectives from clinician-scientists and quality improvement experts Health Sci Rep 2(12) 140 https://doi.org/10.1002/hsr2.140
42. Nayiga S, DiLiberto D, and Taaka L, et al (2014) Strengthening patient-centred communication in rural Ugandan health centres: a theory-driven evaluation within a cluster randomized trial Eval Lond Engl 1995 20(4) 471–491
43. Zhang R, Huang RW, and Gao XR, et al (2018) Involvement of Parents in the Care of Preterm Infants: a Pilot Study Evaluating a Family-Centered Care Intervention in a Chinese Neonatal ICU Pediatr Crit Care Med J Soc Crit Care Med World Fed Pediatr Intensive Crit Care Soc 19(8) 741–747
44. Gálvez M, Zarate A, and Espino H, et al (2017) A short telephone-call reminder improves bowel preparation, quality indicators and patient satisfaction with first colonoscopy Endosc Int Open 5(12) E1172–E1118 https://doi.org/10.1055/s-0043-117954 PMID: 29202000 PMCID: 5698010
45. Ogbuoji O, Geldsetzer P, and Wong C, et al (2020) Impact of immediate initiation of antiretroviral therapy on HIV patient satisfaction AIDS Lond Engl 34(2) 267–276 https://doi.org/10.1097/QAD.0000000000002392
46. Tawfiq E, Desai J, and Hyslop D (2019) Effects of results-based financing of maternal and child health services on patient satisfaction in Afghanistan J Health Serv Res Policy 24(1) 4–10w https://doi.org/10.1177/1355819618802944