Gynaecologic oncology surgical cancellations in Zambia
Samson Chisele1, Mulindi Mwanahamuntu1, Paul Kamfwa2, Mukatimui Kalima-Munalula1, Swali Fundafunda2, Kenneth Chanda1, Maya M Hicks3, Leeya F Pinder4, Krista S Pfaendler5, Groesbeck P Parham1,6 and Michael L Hicks1,6,7
1Department of Obstetrics and Gynecology, University Teaching Hospital – Women and Newborn Hospital, Lusaka 10101, Zambia
2Cancer Diseases Hospital, Lusaka, 10101, Zambia
3Anne Arundel Medical Center, Department of Obstetrics and Gynecology, 2000 Medical Pkwy, Belcher Pavilion, Ste 309, Annapolis, MD 21401, USA
4University of Cincinnati College of Medicine, Ob/Gyn, Cincinnati, OH 45267, USA
5Department of Obstetrics and Gynecology, West Virginia University School of Medicine, 64 Medical Center Drive, Morgantown, WV 26506, USA
6Department of Obstetrics and Gynecology, University of North Carolina at Chapel Hill, 101 Manning Drive, Chapel Hill, NC 27514, USA
7St. Joseph Mercy Oakland Cancer Center, Michigan Cancer Institute, 44405 Woodward Ave, Suite 202, Pontiac, MI 48324, USA
Abstract
Introduction: Cancellations of elective surgery in low-and middle-income countries (LMIC) are common and a major hindrance for patients who are in need of surgical therapeutic modalities. This is especially important in the context of scaling up needed surgical interventions for gynaecological cancer care. There is a knowledge gap in the literature related to cancellation of gynaecologic oncology surgeries in LMIC, where there is enormous need for this specific cancer surgical capacity. We report in an observational descriptive fashion, our experience at the UTH/CDH in Lusaka, Zambia, on the causes of surgical cancellations in gynaecologic oncology.
Methods: From January 1, 2021 through June 31, 2023, we retrospectively evaluated the surgical registry for gynaecologic oncology at the UTH/CDH in Lusaka, Zambia to assess the number and causes of surgical cancellations.
Results: There were a total of 66 (16.96%) surgical cancellations out of 389 scheduled gynaecologic oncology cases. Lack of available blood and/or low haemoglobin was the most frequent cause of surgical cancellations, 27 cases (40.90%).
Conclusion: We highlight in our series that the lack of blood, leading to surgical cancellations was the most frequent impediment related to performing scheduled gynaecologic oncology surgical procedures. As gynaecologic oncology services scale up in LMIC, given the radical nature of surgery and its association with blood loss, it is incumbent on the entire clinical ecosystem to address this issue and to develop mitigating strategies, specific to their respective resource setting.
Keywords: surgical cancellations in LMIC, gynaecologic surgical cancellations in LMIC, blood loss and surgical cancelations in gynaecologic oncology, lack of blood and surgical cancellations
Correspondence to: Samson Chisele
Email: chiseles@gmail.com
Published: 02/11/2023
Received: 22/06/2023
Copyright: © the authors; licensee ecancermedicalscience. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Surgical cancellations for elective surgery in low- and middle-income countries (LMIC) are not uncommon. Reports have evaluated this problem on a broad perspective, inclusive of evaluating social determinants and infrastructural challenges while collectively looking across different surgical service lines [1–8]. These cancellations are a major hindrance for patients required to receive needed surgical care. This is especially important in the context of cancer care where it is predicted that only 5% of patients in LMIC will receive safe, affordable and timely surgery [9].
There appears to be a gap in the literature related to cancellation of surgery specific to the specialty of gynaecologic oncology. This is an important subject to investigate, especially in the context of the World Health Organization’s (WHO) 90/70/90 initiative (WHO November 17, 2020, Global Strategy) to reduce the burden of cervical cancer in LMIC. In sub-Saharan Africa cervical cancer is the leading cause of death among women and the second most common form of cancer [10]. Consistent with the WHO’s initiative, as screening increases in LMIC, it is estimated that up to 50% of these patients will be identified to have early stage, potentially curable disease [11]. For a cure to occur in comporting with the WHO management recommendations, these early-stage lesions require radical cancer surgery, a radical abdominal hysterectomy and pelvic lymphadenectomy. Therefore, identifying the causes of surgical annulment in this environment is extremely important.
At the University Teaching Hospital (UTH) and Cancer Diseases Hospital (CDH) in Lusaka, Zambia, we retrospectively evaluated all cancellations of surgical cases specific to the gynaecologic oncology service. We report here in an observational descriptive fashion our findings and suggest recommendations targeted for future improvements.
Methods
From 1 January 2021 through 31 June 2023 we retrospectively evaluated the surgical registry for gynaecologic oncology at UTH and CDH in Lusaka, Zambia, to assess the number of cases resulting in surgical cancellations. All listed causes of cancellations were identified in order to determine the most prevalent causes of surgical cancellation.
Results
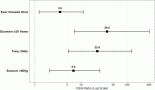
There were a total of 66 (16.96%) surgical cancellations out of 389 scheduled cases for gynaecologic oncology surgeries (Table 1). Causes of surgical cancellation identified are as follows: 27 cases (40.90%) from low haemoglobin and lack of blood, 10 cases (15.15%) were no longer amenable to surgery, 10 cases (15.15%) were cancelled for other reasons not determined from available data sources, 7 cases (10.61%) from unavailable anaesthesiologists, 4 cases (6.06%) from severe uncontrolled hypertension, 3 cases (4.55%) from unavailability of surgeon, 2 cases (3.03 %) from deep vein thrombosis, 2 cases (3.03%) from failed intubation and 1 case (1.52%) from unavailable anaesthetic drugs (Table 2).
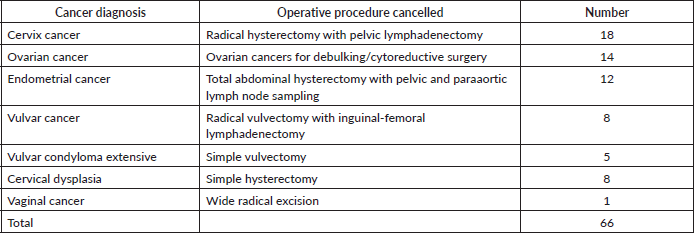
The specific cancers diagnosis and procedures that were cancelled, excluding the two cases of failed intubations, were as follows: 18 stage IB cervix cancers for radical hysterectomy with pelvic lymphadenectomy, 14 ovarian cancers for debulking/cytoreductive surgery, 12 endometrial cancer for total abdominal hysterectomy with pelvic and paraaortic lymph node sampling, 8 vulva cancers for radical vulvectomy with inguinal-femoral lymphadenectomy, 8 persistent high grade squamous Intraepithelial lesion of the cervix for simple hysterectomy, 5 large vulvar condylomas for simple vulvectomy and 1 vaginal cancer for wide radical excision (Table 3).
Table 1. Total number of cases and cancelations.
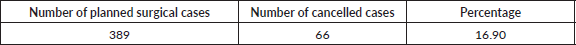
Table 2. Causes and percentage of surgical cancellation.
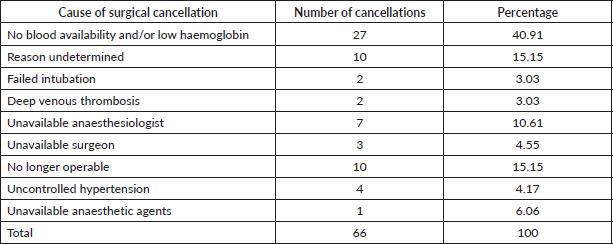
Table 3. Specific cancers diagnosis and procedures that were cancelled.
Discussion
Across surgical service lines in LMIC operative cancellations of scheduled surgical cases range from 18% to 31% [1–8]. Most common causes of reported cancellations were surgeons or anaesthesiologist unavailability; lack of operating theatre time, equipment, ancillary surgical personnel and electricity; and improper surgical scheduling. These important infrastructural and social determinant barriers to surgery in LMIC have been well documented and it was not our intent to readdress these already reported issues. Furthermore, these reports elucidate a void in the literature with no mention of gynaecologic oncology surgery specifically, or link to how these surgical impediments impacts the management of a specific cancer disease entity endemic to LMIC identified by the WHO for eradication. Our study focused specifically on causes of surgical cancellations in gynaecologic oncology. As gynaecologic oncology surgical capacity increases in LMIC in an attempt to achieve the WHO’s initiative, it is important to know specific barriers that potentially will be faced related to surgical cancellations. To our knowledge to date this has not been reported in the literature.
In our series, we report a surgical cancellation rate of 16.96%. This number is slightly lower than the cited rates reported in the literature [1–8]. Although our number of cases is similar to other published reports (146 cases [1], 369 cases [7], 243 cases [8]), this lower rate may be a reflection associated with a specific single surgical oncological service analysis, the fact that we had no documented causes of cancellations related to social determinants such as lack of electricity and fewer cases being cancelled related to lack/absence of professional personnel (surgeon or anaesthesiologist), given that this centre is the only major referral centre for gynaecologic oncology in the entire country [1, 7, 8]
The most common identified reason for surgical cancellations was having a low haemoglobin and/or the lack of blood products (40.90%) being available on the date of scheduled surgery. Lack of blood products were not considered to be the most dominant cause of surgical cancellations in other reported studies; nor was there mention if blood loss was a common associated complication with a proposed oncological surgical procedure [1–8]. In the specialty of gynaecologic oncology this finding is of enormous importance. In LMIC cervical cancer is the second most common malignancy in women, incidence and mortality rates in sub-Saharan Africa are among the highest in the world, and is the leading cause of cancer deaths in women [10]. However, approximately 40%–50% of these patients have potentially preventable deaths secondary to having early stage disease that can be cured with a radical abdominal hysterectomy and pelvic lymphadenectomy [11]. This is why there is a major push to establish traditional and innovative ways to construct gynaecologic oncology surgical capacity in LMIC [12, 13]. However, it is vital to understand the challenges of radical pelvic surgery. A known common complication of this operation is intra-operative blood loss with the average amount being 1 L. This is much more common in LMIC where often these early stage cancer lesions will be much larger and surgery is often the only modality of therapeutic intervention in the absence of radiation and limited chemotherapy. Other gynaecologic oncological operations such as ovarian cancer tumour debulking, radical vulvectomy and inguinal-femoral lymphadectomy for large vulva cancer lesions, large vulva condyloma removals, radical vaginectomy and some nonradical hysterectomies are also associated with significant blood loss. These tumour groups represented the majority of the cancellations in our study. This consequential finding is important to document in the literature for the benefit of our institution and other equivalent LMIC centres in an effort to eliminate this principle impediment to surgical cancellations.
Reported causes of the lack of safe quality available blood in LMIC are attributed to many factors such as: transfusion-transmissible infections (HIV, Hepatitis B&C, malaria and syphilis), lack of benevolent donors, high demand on family donor-ship and lack of public awareness and political will [14, 15] Therefore, from a strategic perspective, while promoting for surgical capacity building in LMIC, it is important for stake holders and policy makers to simultaneously address and make improvements to ensure that these potentially preventable barriers for the availability of safe quality blood are curtailed. Solutions that have been put forth involve education at the local and governmental level related to developing better coordinated blood transfusion services, policies, regulation and legislation as well as expanding the pool of regular unpaid donors and rational use of blood to prevent unnecessary use. These goals and objective are very important and essential to the longevity of a country having safe available blood and the ability to build surgical capacity for gynaecologic malignancies. However, as these initiatives scale up, which we have implemented, in the immediate phases to prevent delays in oncological surgery, the dependency on family donors for current supplies will be essential. So, there will need to be implementation of a better focus on pre-operative assessment strategies to achieve this goal to prevent surgical cancellations.
Weaknesses of this study is that it is retrospective and depends on proper documentation in the cancellation logs of the surgical centre, which is subject to human variability and documentation errors. This is highlighted by the fact ten cases had no documented reason for the cause of delay. Another relative weaknesses is related to the overall number of scheduled surgical cases during the documented study period. This is secondary to the information being exclusively obtained from a single cancer surgical service line, gynaecologic oncology, that is the only referral centre in the country. Nevertheless, our number of surgical cases comports with other reported published series; and we were able to clearly show an important relevant contributing cause of surgical cancellations in gynaecologic oncology. Additionally, another contributing factor of reduced numbers in our series may be related to the COVID-19 pandemic in the 2021 timeframe.
Conclusion
We highlight in our series that the lack of blood, leading to surgical cancellations was the most frequent impediment related to performing scheduled gynaecologic oncology surgical procedures. As gynaecologic oncology services scale up in LMIC, given the radical nature of surgery and its association with blood loss, it is incumbent on the entire clinical ecosystem to address this issue and to develop mitigating strategies, specific to their respective resource setting.
Acknowledgments
Friends of Africa, Inc.
Conflicts of interest
None.
Funding
None.
References
1. Desta M, Manaye A, and Tefera A, et al (2018) Incidence and causes of cancellations of elective operation on the intended day of surgery at a tertiary referral academic medical center in Ethiopia Patient Saf Surg 12 25 https://doi.org/10.1186/s13037-018-0171-3 PMID: 30154916 PMCID: 6109985
2. Ogwal A, Oyania F, and Nkonge E, et al (2020) Prevalence and predictors of cancellation of elective surgical procedures at a Tertiary Hospital in Uganda: a cross-sectional study Surg Res Pract 2020 1464098 PMID: 32258365 PMCID: 7115171
3. Abate SM, Chekole YA, and Minaye SY, et al (2020) Global prevalence and reasons for case cancellation on the intended day of surgery: a systematic review and meta-analysis Int J Surg Open 26 55–63 https://doi.org/10.1016/j.ijso.2020.08.006 PMID: 34568611 PMCID: 7440086
4. Feleke MG, Chichiabellu TY, and Ayalew TL (2022) Magnitude and reasons of surgery cancellation among elective surgical cases in Wolaita Sodo University Comprehensive Specialized Hospital, Southern Ethiopia, 2021 BMC Surg 22 300 https://doi.org/10.1186/s12893-022-01749-y
5. Starr S, Kim WC, and Oke R, et al (2022) The third delay in general surgical care in a Regional Referral Hospital in Soroti, Uganda World J Surg 46 2075–2084 https://doi.org/10.1007/s00268-022-06591-0 PMID: 35618947 PMCID: 9334422
6. Kajja I and Sibinga C (2014) Delayed elective surgery in a major teaching hospital in Uganda Int J Clin Transfus Med 2 1–6 https://doi.org/10.2147/IJCTM.S59616
7. Ayele A, Weldeyohannes M, and Tekalegn Y (2019) Magnitude and reasons for surgical case cancellation at a specialized hospital in Ethiopia J Anesth Clin Res 10(927) 2
8. Egbor P and Edetanlen B (2018) Prevalence and reasons for cancellation of elective oral and maxillofacial surgeries in a tertiary hospital Niger Hosp Prac 22(3–6) 43–47
9. Sullivan R, Alatise O, and Anderson B, et al (2015) Global cancer surgery: delivering safe, affordable, and timely cancer surgery Lancet Oncol 16(11) 1193–1224 https://doi.org/10.1016/S1470-2045(15)00223-5 PMID: 26427363
10. Bray F, Parkin DM, and African Cancer Registry Network (2022) Cancer in sub-Saharan Africa in 2020: a review of current estimates of the national burden, data gaps, and future needs Lancet Oncol 23(6) 719–728 https://doi.org/10.1016/S1470-2045(22)00270-4 PMID: 35550275
11. Parham G, Mwanahamuntu M, and Kapambwe S, et al (2015) Population-level scale-up of cervical cancer prevention services in a low-resource setting: development, implementation, and evaluation of the cervical cancer prevention program in Zambia PLoS One 10(4) e0122169 https://doi.org/10.1371/journal.pone.0122169 PMID: 25885821 PMCID: 4401717
12. Hicks ML, Mutombo A, and YouYou TG, et al (2021) Building workforce capacity for the surgical management of cervical cancer in a fragile, low-income African nation – Democratic Republic of the Congo Ecancermedicalscience 15 1232 https://doi.org/10.3332/ecancer.2021.1232
13. Hicks ML, Mwanahamuntu M, and Butler R, et al (2022) The evolution of a novel approach to building surgical capacity for cervical cancer in Africa ecancer 16 1469 https://doi.org/10.3332/ecancer.2022.1469
14. Osaro E and Charles AT (2011) The challenges of meeting the blood transfusion requirements in Sub-Saharan Africa: the need for the development of alternatives to allogenic blood J Blood Med 2 7–21 https://doi.org/10.2147/JBM.S17194
15. Barro L, Drew VJ, and Poda GG, et al (2018) Blood transfusion in sub-Saharan Africa: understanding the missing gap and responding to present and future challenges Vox Sang 113(8) 726–736 https://doi.org/10.1111/vox.12705 PMID: 30221365