Background: Cervical precancer screening in low-resource settings is largely opportunistic with low coverage. Many women in these settings, where the burden of cervical cancer is highest, only visit health institutions when pregnant or after delivery. We explored screening during antenatal and postnatal visits aimed at increasing coverage.
Methods: Pregnant women (in any trimester) attending antenatal care (ANC) and women attending postnatal care (PNC; 6–10 weeks) clinics were screened at Catholic Hospital, Battor and at outreach clinics from February to August 2022 (08/02/2022 to 02/08/2022). At the same visit, cervical specimens were obtained for high-risk human papillomavirus (hr-HPV) DNA testing (with the Sansure MA-6000 PCR platform) followed by either visual inspection with acetic acid (VIA) or mobile colposcopy with the enhanced visual assessment system.
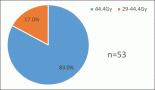
Results: Two hundred and seventy and 107 women were screened in the antenatal and postnatal groups, respectively. The mean ages were 29.4 (SD, 5.4) in the ANC group and 28.6 (SD, 6.4) years in the PNC group. The overall hr-HPV prevalence rate was 25.5% (95% confidence interval (CI), 21.1–29.9) disaggregated as 26.7% (95% CI, 21.4–31.9) in the ANC group and 22.4% (95% CI, 14.5–30.3) in the PNC group (p = 0.3946). Overall, 58.9% of pregnant women (28.3% hr-HPV+) and 66.4% of postnatal women (22.5% hr-HPV+) only visited a health facility when pregnant or after delivery (at Child Welfare Clinics). The VIA ‘positivity’ rate for all screened women was 5.3% (95% CI, 3.1–7.6), disaggregated into 5.2% (95% CI, 2.5–7.8) in the ANC group and 5.7% (95% CI, 1.3–10.1) in the PNC group (p-value = 0.853).
Conclusion: A significant number of women in Ghana only visit a health facility during pregnancy or after delivery. ANC and PNC clinics would offer opportunities to increase coverage in cervical precancer screening in low-resource settings. Relying on community nurses ensures that such programmes are readily integrated into routine care of women and no opportunity is missed.